What are health inequalities?
Health inequalities are the unjust and avoidable differences in people’s health across the population and between specific population groups. Some authors, particularly from North America, use ‘inequalities’ to denote differences between groups and ‘inequities’ to denote unjust differences between groups. The more commonly used term “inequality” has been adopted throughout this website to describe unjust differences.
Health inequalities go against the principles of social justice because they are avoidable. They do not occur randomly or by chance. They are socially determined by circumstances largely beyond an individual’s control. These circumstances disadvantage people and limit their chance to live longer, healthier lives.
The existence of health inequalities in Scotland means that the right of everyone to the highest attainable standard of physical and mental health is not being enjoyed equally across the population.
Examples of health inequalities
In the most affluent areas of Scotland, men experience 23.8 more years of good health and women experience 22.6 more years compared to the most deprived areas.
The life expectancy of people with learning disabilities is substantially shorter than the Scottish average.
Gender-based violence is experienced unequally, with 17% of women and 7% of men having experienced the use of force from a partner or ex-partner at some point in their lives.
The video below shows the extent of health inequalities in Scotland.
You can also watch the full length video on YouTube (external site).
Causes of health inequalities
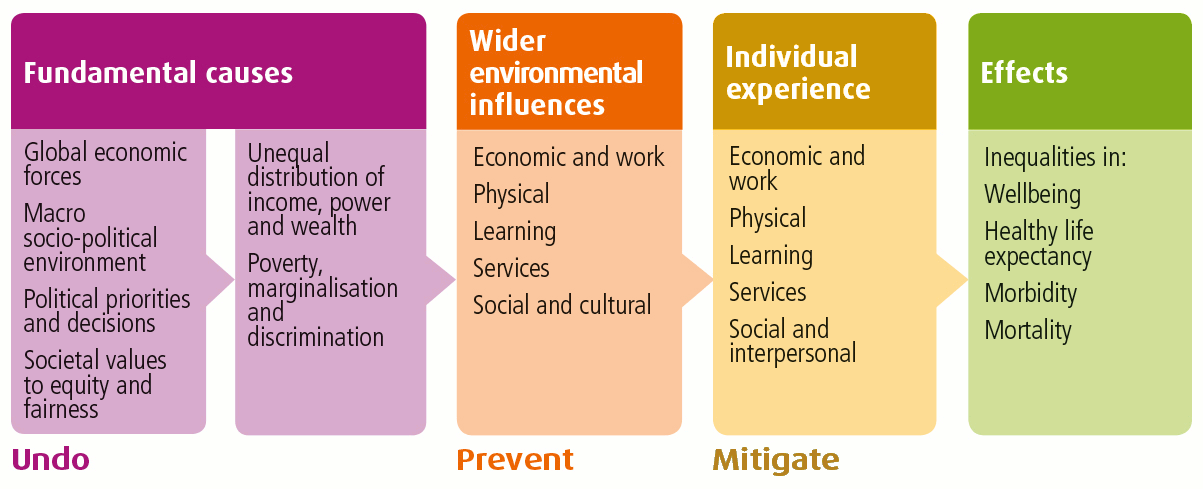
As shown in the diagram above, the fundamental causes of health inequalities are an unequal distribution of income, power and wealth. This can lead to poverty and marginalisation of individuals and groups.
These fundamental causes also influence the distribution of wider environmental influences on health, such as the availability of
- work
- education
- good quality housing.
They can also influence access to services and social and cultural opportunities in an area and in society.
The wider environment in which people live and work then shapes their individual experiences of
- low income
- poor housing
- discrimination
- access to health services.
This environment then shapes individual experiences across the population and leads to the inequalities in health outcomes.
You can find out more about this in our inequality briefing.
National actions
Nationally, the focus should be on implementing the measures which are most likely to be effective in reducing health inequalities. This means trying to discontinue or modify measures which have been shown to widen, or potentially widen, inequalities.
There is also an important role for national agencies, including public and third sector organisations, to support local delivery through advocacy and evidence building.
We examined what does, and does not, work to reduce health inequalities for the Ministerial Task Force on Health Inequalities in 2012. Our Health Inequalities Policy Review shows that tackling health inequalities requires a combination of action to
- undo the fundamental causes
- prevent the harmful wider environmental influences
- mitigate (make less harmful) the negative impact on individuals.
You can find out more about this in our health inequalities policy review which was written to provide evidence to the 2013 Scottish Ministerial Task Force on Health Inequalities. It reviews the current policy and the evidence about what works to address health inequalities.
Local actions
Locally, public resources need to be allocated according to need so that they do not make inequalities worse, and may make a contribution towards their reduction. Providing universal services with added intensive support for vulnerable groups (known as proportionate universalism) is effective at reaching all of those that need them by ensuring that there are fewer or no barriers in terms of
- price
- stigma
- accessibility
- discrimination.
However, some people continue to experience barriers to accessing services, including
- physical
- language
- attitudinal
- information.
These include people from minority ethnic or LBGTI (Lesbian, Gay, Bisexual, Transgender or Intersex) population groups or people living with poverty, disability or mental health problems. Additional efforts are also required to ensure equality of access to services for those living furthest from service provision.
Value cannot be null. Parameter name: source
